пФЧЕФЙФШ
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
Christian Veillette 23 нБТФ 2007, 17:58
|
Alex
What is your indication for surgical management? What kind of fracture do you think it is? It looks like a transverse type although it has been a couple of years since I looked at an acetabular fracture.
Displaced acetabular fractures: indications for operative and nonoperative management.
Tornetta P 3rd. Department of Orthopaedic Surgery, Boston University School of Medicine,
Boston, MA, USA.
Displaced acetabular fractures are a challenging problem. In contradistinction to most conditions in which surgery is based on specific operative indications, displaced acetabular fractures should be considered an operative problem unless specific criteria for nonoperative management are met. These include a congruent hip joint on the anteroposterior and oblique (Judet) radiographs, an intact weight-bearing surface (as defined by roof arc and subchondral arc measurements on computed tomographic scans), and a stable joint. The final decision about the treatment method must also consider the patients functional demands, expectations, and physical condition and the physicians experience and institutional support for dealing with this type of injury. Displaced both-column fractures with secondary congruence may have better results than other displaced fractures.
In older patients, nonoperative management may be effectively utilized.
Understanding the current criteria for effective use of nonoperative treatment will help the surgeon make these difficult decisions.
J Am Acad Orthop Surg. 2001 Jan-Feb;9(1):18-28.
http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?db=pubmed&cmd=Retrieve&dopt=Ab
stractPlus&list_uids=11174160&query_hl=5&itool=pubmed_docsum
Can you improve the reduction at this stage or will you end up with an OIF (Open internal fixation) and leave it malreduced?
Delayed reconstruction of acetabular fractures 21-120 days following injury.
Johnson EE, Matta JM, Mast JW, Letournel E.
Department of Orthopaedic Surgery, University of California, Los Angeles
90024.
A retrospective review was performed of 207 patients treated by delayed reconstruction of acetabular fracture between 21 and 120 days following injury. Nineteen patients were lost to followup. One hundred eighty seven patients had 188 fractures classified as follows; 35 posterior wall, 9 posterior column, 5 anterior wall, 4 anterior column, 13 transverse, 49 transverse/posterior wall, 21 T shape, 8 posterior column/posterior wall, 8 anterior column posterior hemitransverse, and 34 both column fractures. The
average preoperative delay was 43 days. Followup averaged 6.5 years (range, 9 months-30 years). Overall good to excellent results were achieved in 65% of patients, fair in 9%, and poor in 26%. Good to excellent results by fracture type were; posterior wall (51%), posterior column (89%), anterior wall (60%), anterior column (100%), transverse (69%), transverse/posterior wall (59%), T shape (62%), posterior column/posterior wall (88%), anterior column/posterior hemitransverse (75%), and both column (72%). Heterotopic ossification developed in 49 of 168 patients without prophylactic treatment, in 6 of 12 treated prophylactically with diphosphonate, and in 2 of 27 receiving prophylactic indomethacin therapy. There were 20 postoperative sciatic nerve palsies, 3 immediate and 5 delayed infections, 5 cases of
pulmonary embolism, and 26 cases of avascular necrosis. Delayed management
of acetabular fractures increases the difficulty of operative treatment and may result in a significant reduction in good to excellent results. Simple anterior or posterior wall fractures, associated transverse + posterior wall
fractures, and T shape fractures have an increased risk of failure when treated within this time period.
Clin Orthop Relat Res. 1994 Aug;(305):20-30.
http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?db=pubmed&cmd=Retrieve&dopt=Ab
stractPlus&list_uids=8050229&query_hl=3&itool=pubmed_DocSum
My concern would be that the risk of leaving it malreduced is very high. It appears to be primarily a gap rather than a step in the articular surface. Do you have any CT views that show an articular step?
Regards
Christian
****************************************
Christian Veillette M.D., FRCSC, M.Sc., B.Sc.(Hon)
Upper Extremity Reconstruction & Trauma Fellow
|
[
пФЧЕФЙФШ ]
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
Dr.A.K.Venkatachalam 24 нБТФ 2007, 18:42
|
Hello,
I would do a ORIF through an ilioinguinal approach with a long recon plate.
REduciton may not be difficult, you can apply intraop traction to the head through a lateral pin in the neck and head of the femur to reduce the fractures. Also the supra acetabular fracture needs to be fixed through a iliac approach osteotomiisng the iliac crest and applying any plate.
with best regards
Dr.A.K.Venkatachalam
MS, DNB, FRCS, MCh Orth( Liverpool)
Consultant Orthopedic surgeon
Chennai
|
[
пФЧЕФЙФШ ]
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
Christian Veillette 24 нБТФ 2007, 18:49
|
The last two images from the 3-D CT scan certainly makes the fracture look worse than the plan radiographs.
Might have to reconsider my suggestion to leave it alone at this stage.
Ilioinguinal approach would be the best to approach and clean out fracture with recon plate fixation as suggested by Dr. Venkatachalam.
I would be interested to hear what one of the pelvic/acetabular fracture surgeons like Dr. Routt on the OTA list would recommened.
Regards
Christian
|
[
пФЧЕФЙФШ ]
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
Chip Routt 24 нБТФ 2007, 21:05
|
The joint is non-concentric as the head appears to be either "following the caudal segment", or the dome component is displaced from the tethered head... or so it seems... and he's young... so, many fracture surgeons would recommend reduction and fixation.
So we must decide preoperatively which part is the displaced segment?
It's difficult to know from these few selected images which component of the injury (was before and now) should be deemed the "soon to be mobile"
segment. It's my best guess that it is the caudal portion and there exists a healing fracture line somewhere thru the posterior column...one image
suggests it. If true, its early healing/union should be disrupted, and the resultant fragment mobility then allows accurate reduction.
Such work is not always possible using a single exposure... it's not unreasonable to first access the healed zone and osteotomize it using one direct exposure, then turning the patient if necessary to use another opposite exposure to further mobilize the fracture, reduce, clamp, and fix it.
On the other hand, some surgeons advocate an extended iliofemoral exposure for these scenarios. For a variety of reasons, I've never been much of a fan.
In summary, reduction and fixation would be good. If you have an excellent 3D brain, a quality OR fluoroscopy unit, and are slick with an osteotome and clamps thru the ilioinguinal exposure then you've made your best choice.
Remember that the symphysis is the caudal segment's "hinge" and may need destabilizing as well if it's affecting the reduction adversely.
If you have other images which cause you to decide to destabilize the posterior column fracture component using a direct or EIF exposure, then you
have better info than we can see.
Or you can just leave it... he has good dome coverage and it may be a durable hip for some time... maybe.
Chip
M.L. Chip Routt, Jr.,M.D.
Professor-Orthopedic Surgery
Harborview Medical Center
|
[
пФЧЕФЙФШ ]
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
пФРТБЧЙФЕМШ: Frederic B. Wilson, M.D. 25 нБТФ 2007, 00:17
|
Chip, et al.,
While not claiming to have the best 3D brain around, it appears to me from the limited images available, that the caudal segment is stable from the symphysis to the SI joint on the fracture side. I would love to see the rest of the transverse CT images to see where the fracture line actually exits posteriorly on both the inner and outer tables of the ilium. In my hands,
assuming that the femoral head has followed the cephalad (dome) fragment, I would use an ilioinguinal approach and take down the fracture line from anterior to posterior, distracting with a lamina spreader, if necessary, to clean out and inspect the joint. I would then reduce the cephalad fragment to the caudal fragment using jungbluth or farabeuf clamp and screws and then apply a plate and screws. If the fracture exits posteriorly would you then favor an additional posterior approach to clean out and reduce from that side?
My concept is that what I am after is restoring the anterior portion of the acetabular ring to the superior dome portion to re-establish the containment of the femoral head in an intact "horseshoe". Is this accurate?
Best regards,
Fred
Frederic B. Wilson, M.D.
Assistant Professor
Trauma and Adult Reconstruction
Department of Orthopaedic Surgery
Louisiana State University Health Sciences Center
2020 Gravier St., #728
New Orleans, Louisiana, 70112
|
[
пФЧЕФЙФШ ]
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
пФРТБЧЙФЕМШ: Chip Routt 26 нБТФ 2007, 13:32
|
Who knows? The images are insufficient to detail a reasonable plan.
|
[
пФЧЕФЙФШ ]
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
пФРТБЧЙФЕМШ: Alexander Chelnokov 27 нБТФ 2007, 08:14
|
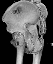
Some more images. Does it help to guess which part of the acetabulum is displaced?
|
[
пФЧЕФЙФШ ]
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
пФРТБЧЙФЕМШ: Chip Routt 27 нБТФ 2007, 08:18
|
Normal appearing SI joints and a healed posterior column limb... my bet's on caudal segment displacement.
MLCR
|
[
пФЧЕФЙФШ ]
|
Re: оЕМЕЮЕООЩК РЕТЕМПН ЧЕТФМХЦОПК ЧРБДЙОЩ
пФРТБЧЙФЕМШ: Dr Abdelsalam EID 25 нБТФ 2007, 11:43
|
Dear Alexander
Chip Routt wrote:
........................
Or you can just leave it...he has good dome coverage and it may be a durable
hip for some time...maybe.
I would totally recommend leaving him alone.
The anterior element of the fracture is so low and the anterior roof arc angle must be at least 60 deg.
The posterior element is so minmally undisplaced. There is good congruence of the joint, and to top it all, 6 weeks have passed. If you consider ORIF now, I don't expect that much improvement could be accomplished. Not to mention the need for extensive approaches with their morbidity.
If you leave him alone now, and if the need arises in the future I believe that a standard THR would be good enough. And this is of course a much simpler procedure than the ORIF currently considered.
Dr Abdelsalam EID M.D., AFSA (Paris V)
AO Fellow
Lecturer of Orthopedic Surgery
Faculty of Medicine, Zagazig University,
Egypt.
|
[
пФЧЕФЙФШ ]
|
|
( пФЧЕФЙФШ )
|
|